- Search
| Ann Rehabil Med > Volume 43(1); 2019 > Article |
|
Abstract
Objective
To determine anatomical variation of the sural nerve (SN) by ultrasonography (US) and compare sensory nerve action potential (SNAP) of the SN obtained by a control method to that obtained with adjusted method using US.
Methods
Eighty legs of 40 healthy volunteers were enrolled. The location and formation of SN were investigated through US. Two methods of nerve conduction study (NCS) were then performed. In the control method, the cathode was placed 14 cm proximal to the lateral malleolus and the greatest SNAP amplitude was obtained by moving the cathode medially or laterally from just lateral to the calf-mid line. In adjusted NCS, the exact SN union site was stimulated in type 1. In other SN types, the stimulation was done directly over the nerve and the distance from the lateral malleolus was set to be 14 cm.
Results
It was found that 73.8% of the SNs were type 1, 22.5% were direct continuation of MSCN (type 2), and 3.8% were MSCN and LSCN without communicating (type 4). However, type 3 was not found. The union point in type 1 SN was 12.6±2.5 cm proximal to the lateral malleolus and 1.4±0.7 cm lateral to the calf-midline. After stimulation adjustment, SNAP amplitude in type 1 SN was significantly increased (20.7±5.5 μV vs. 27.1±6.7 μV).
The sural nerve (SN) is one of the sensory nerves in the lower limb supplying skin of the lateral and posterior part of the inferior third of the leg and the lateral side of the foot. The SN is known to originate just distal to the popliteal fossa. It is formed by union of the medial sural cutaneous nerve (MSCN, a branch of the tibial nerve) and the lateral sural cutaneous nerve (LSCN, a branch of the common fibular nerve) [1]. The site of union of the MSCN and LSCN to form SN is highly variable, usually in the distal third of the leg, but also in the popliteal fossa or at the ankle rarely [2].
Understanding the anatomy of SN is clinically important for numerous situations such as nerve conduction studies (NCS), nerve biopsies, and nerve graft procedures. In electrodiagnostic studies, the sural NCS is very useful for the diagnosis of generalized peripheral neuropathy or focal neuropathy including lumbosacral plexopathy, sciatic neuropathy, and tibial neuropathy. Many laboratories and multiple international studies have used a distance of 14 cm from the recording electrode for stimulation with antidromic technic [3,4]. However, anatomical variations of SN such as their types of nerve formation, course, and union site can cause improper stimulation of the SN and result in different parameters of the sensory nerve action potential (SNAP), ultimately leading to misinterpretation of electrodiagnostic findings [5]. Several precedent researches have evaluated the correlation between anatomical variation and NCS in the SN. Needle electrodes have been used in these ultrasound-guided NCS studies [6]. However, rather than needle electrodes, surface electrodes are mainly used in clinical practice because they give us more information and they are easier to apply. One previous study has tried to find the optimal stimulation site in sural NCS by varying the distance from the midcalf based on ultrasonographic findings [5]. It would be also meaningful to analyze sural NCS results by varying the stimulation distance from the lateral malleolus.
Thus, the objective of this study was to investigate types of the SN formation through ultrasonography (US) and conduct adjusted sural NCS with surface electrode based on sonographic findings. The SN was directly stimulated under US and adjustment in stimulation site was made bi-directionally: not only horizontally from calf-midline, but also vertically from the lateral malleolus.
Ultrasonographic examinations were performed on 80 legs of 40 healthy subjects from 2016 to 2017. Subjects were excluded if they had history of lower limb trauma, surgery, leg deformity, known peripheral polyneuropathy, or any medical conditions that could accompany peripheral polyneuropathy. General characteristics such as age, sex, height, weight, body mass index (BMI), and leg length were evaluated. Leg length was measured from the prominence of lateral malleolus to the midpoint of popliteal crease with prone position. All subjects provided informed consent documentation. This study was approved by Institutional Review Board of Korea University Guro Hospital (No. 2016GR0234).
Ultrasonographic study and NCS were performed by a single skilled physiatrist with more than 10 years of experience. In the ultrasonographic study, a HD15 system (Philips Healthcare, Bothell, WA, USA) with a 7–12-MHz linear array transducer was used. All participants were placed in prone position with knees fully extended and ankle in neutral position. The examination began from the distal one quarter of the leg and traced the SN upward to confirm the joining of MSCN and LSCN. By observing the whole SN, its formation type was identified. Based on previous studies, SN formation was divided into the following types: type 1, classical pattern (union of MSCN and LSCN); type 2, extending from MSCN alone; type 3, extending from LSCN alone; type 4, MSCN and LSCN are separate and running parallel to each other down to the ankle [5] (Fig. 1). Symmetrical distribution of SN type (i.e., whether bilateral legs have the same type of SN) was also checked. In type 1 SN formed by union of MSCN and LSCN, the union point was recorded by measuring two distances: the vertical distance to the most prominent part of the lateral malleolus (means SN length) and the horizontal distance to the midcalf line connecting the calcaneal tendon and the middle of the popliteal fossa (Fig. 2). Two methods of NCS were then performed in all SNs with antidromic technic. Control NCS of SN was carried out in the same posture as described above. An active electrode (E1) was placed behind the most prominent part of the lateral malleolus at the midpoint between the lateral malleolus and the Achilles tendon while the reference electrode (E2) was placed 4 cm distal to E1. Afterwards, 14 cm proximal to the most prominent point of lateral malleolus was stimulated. By moving the cathode medially or laterally from lateral to the calf-mid line, the largest SNAP amplitude was found. The stimulation was conducted in supra-maximal intensity ranging from 10 to 50 mA (duration, 0.2 ms). In adjusted sural NCS, the stimulation site was made depending on the type of SN formation. For type 1 SN, the exact union site recorded by US was stimulated. However, when the SN length was longer than 14 cm, the adjusted nerve stimulation was done at 14 cm proximal to the lateral malleolus rather than at the union site. For types 2 and 3 SNs, the stimulation was done directly over the nerve through US and the distance from the lateral malleolus was also set to be 14 cm. For type 4 SN, separately stimulating MSCL and LSCN was tried and the largest amplitude was recorded.
For statistical analysis, SPSS version 22.0 for Windows (IBM Inc., Armonk, NY, USA) was used. Bilateral SN features such as SN length and control SNAP amplitude were compared using Mann-Whitney test. Wilcoxon signed rank test was carried out to compare sural NCS parameters between the control method and the adjusted method. A p-value of less than 0.05 was considered statistically significant.
Detailed characteristics of study subjects and their SNs are summarized in Table 1. The mean height and SN length of females were shorter than those of males. Leg length was shorter in the older group than that in the younger group for both sexes. Sural SNAP amplitudes with control method in older males were significantly smaller than those in younger males (p=0.03, Mann-Whitney test).
The SN was identified in all 80 lower limbs by using US. According to its course and union site, the SN was assorted into four types as mentioned above. In this study, among 80 legs, 59 SN complexes were type 1 (73.8%), 18 SN were type 2 (22.5%), and 3 cases were type 4 (3.8%). Type 3 was not found in this study. The mean nerve length (the distance from the union site to the most prominent part of the lateral malleolus) was 12.6±2.5 cm (range, 8.5–19 cm) and the ratio to the leg length was 32.3%. The mean distance from the union site to midcalf line was 1.4±0.7 cm (Table 2).
In control NCS, the largest SNAP was found by moving the cathode horizontally at 14 cm proximal to the lateral malleolus. Responses were observed in every attempt. The stimulating site was about 1.3±0.9 cm from the midcalf line. When comparing bilateral SN features by using Mann-Whitney test, there was no significant difference in type 1 SN length or control SNAP amplitude (Table 3). In this study, symmetrical distribution of SN formation was observed in 24 (60.0%) out of 40 subjects.
When conducting adjusted NCS under US, in type 1 SN, the union site was 12.6±2.5 cm from the lateral malleolus and 1.4±0.7 cm from the midcalf line. In other types, the stimulation was made 14 cm from the lateral malleolus. The mean distance from the midcalf line was 0.5±0.3 cm in type 2 and 1.0±0.2 cm and 2.1±0.7 cm in type 4 of MSCN and LSCN, respectively. Average distances between control and adjusted stimulation sites were as follows. In type 1 SN shorter than 14 cm, the vertical distance was 2.8±1.3 cm and the horizontal distance was 1.6±0.9 cm. In type 1 SN longer than 14 cm, the distance was 1.3±0.5 cm, 0.2±0.2 cm in type 2 SN, and 0.8±0.2 cm in type 4 SN.
When comparing results of adjusted NCS to control NCS, type 1 SN showed significant difference in SNAP amplitudes compared to other types. When type 1 SNs were divided into two groups according to SN length of 14 cm, there were 37 limbs with SN length shorter than 14 cm and 22 limbs with SN length longer than 14 cm. Both groups showed significant differences between control and adjusted SNAP amplitudes (Table 3). In other types of SN, the difference in amplitudes between the two NCS methods was not statistically significant. In overall type 1 SN, the mean amplitude and peak latency of SNAP by control NCS were 20.7±5.5 μV and 3.1±0.3 ms, respectively. In adjusted NCS, the mean amplitude and peak latency were 27.1±6.7 μV and 2.8±0.4 ms, respectively. The mean SNAP duration using control method (1.40±0.16 ms) and that of using adjusted method (1.37±0.19 ms) showed no significant difference (Table 4).
The SN is of great clinical significance. It plays a major role in diagnosing sensory axonal loss in distal neuropathies. Because of its long length, SNAP can be a sensitive indicator of mild peripheral neuropathy attributable to metabolic disease and other length-dependent peripheral neuropathies. Therefore, knowing its anatomical variation and location can help conduct NCS test more accurately. There have been many studies on this subject by dissecting cadavers or using US [7]. In various studies, the SN formation type was classified into three to as many as six types. Basically, SN consists of LSCN and MSCN, branches of common peroneal nerve and tibial nerve, respectively. When there is variation in the branch, peroneal communication nerve from LSCN can be combined in SN formation. Common peroneal nerve or tibial nerve itself can also directly participate in SN formation without making branches [8-10]. However, because this study was focused on SN formation location, there was relatively less interest in exact origin of SN. In addition, simple classification from previous studies was used [5]. In this study, the SN anatomy adhered to basic principles. It was categorized into four patterns as mentioned above. Our results were similar to previous ones except that type 3 SN was not detected in the present study. This might be due to the small diameter of MSCN and LSCN. The possibility of missing these nerves cannot be ruled out. Moreover, according to previous studies, type 3 SN was identified only in few cases if not found at all [11]. For example, Pyun and Kwon [5] have verified the variation of SN formation through cadaver study and found 20 out of 26 legs of type 1, 4 cases of type 2, and 2 cases of type 4. They did not find type 3 in 26 cadavers either.
Unlike other types of SN, type 1 SN is a union of LSCN and MSCN. It can be more influenced by improper stimulation in NCS depending on union location. Thus, we evaluated union site of type 1 SN by ultrasound. The length of the actual SN formed by the merging of LSCN and MSCN was 12.6±2.5 cm. It was shorter than the length of 14 cm usually used in the control NCS method. We found that the actual length of the SN was proportional to the length of the leg (about 31% for leg length). This has been confirmed by other studies [8,12].
As expected, by knowing the exact location where the SN starts, significant increment of SNAP amplitude is found in ultrasound-guided NCS compared to the control one in type 1 SN. At the same time, peak latency shortened. This was predictable because the average distance from the stimulation site to recording site (EI) was shorter in ultrasound-guided method. However, the increment of SNAP amplitude in the adjusted method was greater than that reported in a previous study [13]. In the previous study that tried to find the reference value for sural SNAP parameters with antidromic NCS method, the ratio of the amplitude in different stimulation distances (14 cm and 12 cm) was 1.10 [13]. Compared to the previous study, the average difference in stimulating distances in the present study was smaller than that in the previous study. However, the difference in amplitude was greater in the present study (about 135%). For one subject, the actual SN length was 12.5 cm and the SNAP amplitude was about twice that of the control method (34.5 μV vs. 17.2 μV). In addition to the short stimulating distance, there are several other reasons for this larger increment in SNAP amplitude. First, more accurate location of SN can be stimulated by using US. In type 1 SNs longer than 14 cm, the average SNAP amplitude by adjusted method was greater than that of the control method. This implies that SN stimulation is more accurate under US. Even with the same vertical stimulation distance of 14 cm, larger SNAP amplitude was obtained in one method compared to the other. Second, summation effect of MSCN and LSCN obtained by stimulating the union site of type 1 SN might have affected the result.
In types 2 and 4 SNs, although SNAP amplitude showed tendency to increase with adjusted NCS method, there was no statistically significant difference between the two NCS methods. Based on results of this study, there is advantage of using US in sural NCS for type 1 SN.
This study has several limitations. First, the increment of SNAP amplitude in adjusted method might be due to summation of MSCN and LSCN and the exact stimulation of SN through US. However, the exact portion of contribution of these two factors remains unknown. Thus, more research would be needed for more accurate comprehension. Second, the number of subjects in this study was relatively small. The lack of observing type 3 SN might be due to such small number. In addition, the number of type 4 SN was small (n=3). This might have been too small to show significant difference between the two NCS methods. Taken these factors into account, further study with larger sample size would be needed. Moreover, most subjects had relatively short height considering the average height of Korean. It could have affected the mean distance from E1 to union site of the SN which is proportional to the length of the leg. Lastly, this study did not include enough people with age of 60s. According to a previous study, age group of 60 and over shows reduction in SNAP amplitude compared to other age groups [14]. A normal age-dependent loss of axons or higher prevalence of unrecognized polyneuropathy in elderly people might be the cause [14].
In pathologic conditions where temporal dispersion and axonal loss occur more prominently, improper stimulation can lead to distinct reduction in SNAP amplitude and conduction velocity which can finally lead to misinterpretation of electrodiagnostic findings [15]. Therefore, US-guided sural NCS can be useful when it is difficult to identify the sural SNAP when the amplitude is small. Moreover, US-guided NCS would be helpful if the patient is in a condition that makes it difficult to compare the sural SNAP with the contralateral side.
In summary, anatomical variations of the SN were examined by US. In addition to anatomical variation, individual difference in height could also affect results when conducting sural NCS. This suggests that using a single cutoff value for establishing normal sural SNAP in fixed stimulation site can cause errors. Therefore, US should be considered as a complementary tool when performing sural NCS for better precision.
ACKNOWLEDGMENTS
This work was supported by the Electronics and Telecommunications Research Institute (ETRI) grant funded by the Korean government (No. 18ZR1230, Research on Beam Focusing Algorithm for Microwave Treatment).
Fig. 1.
Types of sural nerve formation: type 1, classical pattern (union of MSCN and LSCN); type 2, extending from MSCN alone; type 3, extending from LSCN alone; type 4, MSCN and LSCN are separate and running parallel to each other down to the ankle. SCN, sciatic nerve; CPN, common peroneal nerve; TN, tibial nerve; MSCN, medial sural cutaneous nerve; LSCN, lateral sural cutaneous nerve; SN, sural nerve.

Fig. 2.
Sural nerve conduction study with adjusted stimulation location and ultrasonography of a transverse view of sural nerve. (A) Traced upwardly from B level where MSCN and LSCN are just about to divide. (B) Level of ankle. MSCN, medial sural cutaneous nerve; LSCN, lateral sural cutaneous nerve; V, small saphenous vein; E1, active electrode; E2, reference electrode.
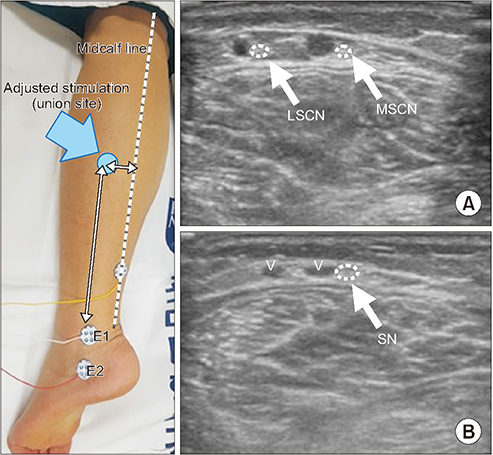
Table 1.
Characteristics of study subjects and SN according to gender and age group
|
Male (n=15) |
Female (n=25) |
Total (n=40) | |||
|---|---|---|---|---|---|
| Younger (n=11) | Older (n=4) | Younger (n=14) | Older (n=11) | ||
| Height (cm) | 175.2±6.0 | 171.0±6.8 | 160.3±4.8 | 161.7±5.2 | 165.8±1.3 |
| Weight (kg) | 71.4±7.5 | 71.5±2.9 | 53.5±6.2 | 57.4±10.4 | 61.3±1.8 |
| BMI (kg/m2) | 23.2±1.7 | 24.5±1.8 | 20.8±2.5 | 22.0±4.3 | 22.19±0.5 |
| Leg length (cm) | 41.8±2.9 | 39.8±3.1 | 39.9±2.7 | 36.8±2.4 | 37.9±3.5 |
| SN lengtha) (cm) | 13.0±2.5 | 13.1±2.1 | 12.0±1.4 | 12.1±2.0 | - |
| SN type (n=80) | |||||
| Type 1 | 17 | 6 | 19 | 17 | - |
| Type 2 | 4 | 2 | 7 | 5 | - |
| Type 3 | - | ||||
| Type 4 | 1 | 2 | |||
| SNAP amplitude | |||||
| Control | 20.1±4.5 | 15.1±3.1 | 21.3±6.2 | 21.9±5.1 | - |
| Adjusted | 23.8±5.6 | 22.0±5.2 | 31.1±6.4 | 26.1±5.5 | - |
Table 2.
Ultrasonographic findings of SN formation types and features of SN
Table 3.
Characteristics of SN and right-left difference in study subjects
| Right leg (n=40) | Left leg (n=40) | Total (n=80) | |
|---|---|---|---|
| SN type | |||
| Type 1 | |||
| ≥14 cm | 10 | 12 | |
| <14 cm | 22 | 15 | |
| Type 2 | 7 | 11 | |
| Type 4 | 1 | 2 | |
| SN lengtha) (cm) | 12.2±2.2 | 12.7±2.0 | |
| SNAP amplitude (μV) | |||
| Control method | |||
| Type 1 | |||
| ≥14 cm | 20.9±8.1 | 24.7±7.4 | 19.2±6.4* |
| <14 cm | 21.5±4.7 | 23.5±5.0 | 22.4±4.5** |
| Type 2 | 17.9±5.2 | 18.5±3.8 | 18.2±4.3 |
| Type 4 | 19 (n=1) | 20.1±5.7 | 19.7±4.1 |
| Adjusted method | |||
| Type 1 | |||
| ≥14 cm | 24.7±7.4 | 22.8±5.2 | 23.7±6.1* |
| <14 cm | 28.4±6.1 | 32.1±4.9 | 30.1±5.8** |
| Type 2 | 17.8±5.5 | 19.6±3.5 | 18.7±4.4 |
| Type 4 | 19.4 (n=1) | 20.5±5.0 | 20.1±3.6 |
REFERENCES
1. Moore KL, Dalley AF. Clinically oriented anatomy. 4th ed. Philadelphia: Lippincott Williams & Wilkins; 1999.
2. McMinn RM. Last’s anatomy: regional and applied. 8th ed. Edinburgh: Churchill Livingstone; 1990.
3. Schuchmann JA. Sural nerve conduction: a standardized technique. Arch Phys Med Rehabil 1977;58:166-8.

4. Buschbacher RM. Sural and saphenous 14-cm antidromic sensory nerve conduction studies. Am J Phys Med Rehabil 2003;82:421-6.


5. Pyun SB, Kwon HK. The effect of anatomical variation of the sural nerve on nerve conduction studies. Am J Phys Med Rehabil 2008;87:438-42.


6. Scheidegger O, Kuffer AF, Kamm CP, Rosler KM. Reproducibility of sensory nerve conduction studies of the sural nerve using ultrasound-guided needle positioning. Muscle Nerve 2011;44:873-6.


7. Kim KH, Yoo JY, You BC. Ultrasonographic evaluation of sural nerve for nerve conduction study. Ann Rehabil Med 2014;38:46-51.



9. Vuksanovic-Bozaric A, Radunovic M, Radojevic N, Abramovic M. The bilateral anatomical variation of the sural nerve and a review of relevant literature. Anat Sci Int 2014;89:57-61.


10. Popieluszko P, Mizia E, Henry BM, Pekala PA, Sanna B, Roy J, et al. The surgical anatomy of the sural nerve: an ultrasound study. Clin Anat 2018;31:450-5.


11. Shankar N, Selvam RP, Dhanpal N, Reddy R, Alapati A. Anatomical variations of the sural nerve in the leg: a fetal study. Neurol India 2010;58:24-8.


12. Coert JH, Dellon AL. Clinical implications of the surgical anatomy of the sural nerve. Plast Reconstr Surg 1994;94:850-5.


13. Sreenivasan A, Mansukhani KA, Sharma A, Balakrishnan L. Sural sensory nerve action potential: A study in healthy Indian subjects. Ann Indian Acad Neurol 2016;19:312-7.



- TOOLS
-
METRICS

- Related articles in ARM
-
Proximal Peroneal Nerve Conduction Study1996 June;20(2)
The Significance of the Area as a Parameter in Nerve Conduction Study1988 December;12(2)
Magnetic stimulation in sciatic nerve conduction study.1993 March;17(1)
Superficial Peroneal Nerve Conduction Study.1997 April;21(2)






