The Efficacy of Physical Therapy to Alleviate Symptomatic Thoracic Radiculopathy: A Systematic Review and Meta-Narrative Analysis
Article information
Abstract
To evaluate the efficacy of physical therapy (PT) to alleviate symptomatic thoracic radiculopathy (TR) without the use of invasive procedures. Database search was conducted by an experienced medical librarian from inception until January 27, 2023, in EBSCO CINAHL with Full Text, Ovid Cochrane Central Register of Controlled Trials, Ovid Embase, Ovid MEDLINE, Scopus, and Web of Science Core Collection. Inclusion criteria included studies that involved adult patients (age≥18) who had a magnetic resonance imaging-confirmed TR and underwent a structured, supervised PT program of any length. All types of studies were included. Study quality and risk of bias were assessed using the National Heart, Lung, and Blood Institute (NHLBI) Study Quality of Assessment Tool. Certainty in evidence was assessed using the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) approach. A meta-analysis was not performed. A total of 1,491 studies were screened and 7 studies met inclusion criteria, 5 case studies and 2 cohort studies. All studies showed improvement or resolution of the TR with PT. Quantitative improvements were not noted in most studies and PT regimens were sparsely described. Overall quality assessment demonstrated 3 studies had “good,” 1 “fair,” and 3 “poor” quality evidence. Certainty of evidence was “low” due to risk of bias. A dedicated PT program may help to alleviate symptomatic TR; however due to limited evidence, risk of bias, and low certainty in evidence, the data is too weak to support a definite conclusion.
INTRODUCTION
Thoracic radiculopathy (TR) is commonly characterized by direct anatomic compression or irritation of exiting spinal nerve roots in the thoracic spine. Clinically it presents with localized pain or paresthesia in the back, chest, or abdomen that follows a dermatomal pattern corresponding to the affected spinal level [1]. Truncal or abdominal muscle weakness in a myotomal distribution may be present [1]. TR pain represents approximately 5% of outpatient pain clinic referrals [2]. Thoracic disc disease specifically is involved in only 0.15%–4% of symptomatic disc herniations of the spine and they represent <2% of all spinal disc surgeries performed [1].
The treatment for TR varies greatly depending on the etiology. Initial conservative treatment with rest and oral analgesics is often recommended. If symptoms progress or conservative measures fail, percutaneous interventional pain control modalities or surgical decompression may be considered. There is limited data available on the treatment of TR solely with physical therapy (PT); however, PT modalities such as dynamic stretching, manual therapy, and postural training have gained recognition as potentially effective management options [3].
To ensure evidence-based recommendations exist and are provided to patients, this systematic review aims to evaluate the efficacy of PT to alleviate symptomatic TR without the use of invasive procedures. The authors seek to contribute to the existing body of medical knowledge and inform clinical practice in the management of this condition as this is the first systematic review and meta-narrative analysis regarding this topic.
METHODOLOGY
Study protocol
Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) guidelines were followed when performing this systematic review [4]. The protocol was submitted in the International Prospective Register for Systematic Reviews (PROSPERO) database on February 7, 2023. It was registered with the most recent edit on February 18, 2023, under the following ID number, CRD42023397753 [5].
Search strategy
The literature was searched by a medical librarian for the concepts of TR and PT. Search strategies were created using a combination of keywords and standardized index terms. Searches were run on January 27, 2023, in EBSCO CINAHL with Full Text (1963+), Ovid Cochrane Central Register of Controlled Trials (1991+), Ovid Embase (1974+), Ovid MEDLINE (1946+ including epub ahead of print, in-process & other non-indexed citations), Scopus (1788+), and Web of Science Core Collection (Science Citation Index Expanded 1975+ & Emerging Sources Citation Index 2015+). After removing pediatric studies based on the exclusion criteria, a total of 2,148 citations were retrieved. One additional text was found independently. Duplicates were removed using Covidence (Covidence systematic review software; Veritas Health Innovation, available at www.covidence.org) leaving 1,491 citations. Full search strategies are provided in Supplementary Table S1.
Study selection process
Studies were selected for our paper if they included adult patients (age≥18) who had an magnetic resonance imaging (MRI)-confirmed TR and underwent a structured, supervised PT program of any length. All types of studies were included. Studies were excluded if they involved children (age<18) or adults without an MRI-confirmed TR. They were also excluded if the patients underwent advanced interventional procedures including but not limited to epidural steroid injections, laminectomies, disc decompressions, spinal cord stimulators, and/or radiofrequency ablations alone or prior to a PT regimen.
In the first phase of the systematic review, each title and abstract identified by the expert librarian were evaluated in duplicate by two of the four independent reviewers (K.A.M., P.T.D., J.P., J.D.H.). Disagreements at this phase were resolved between the two reviewers and a third independent reviewer from the same group via consensus. In the second review phase, two of the same four independent reviewers then screened the full texts of each study procured by the first phase. The full texts were reviewed in duplicate, and disagreements were resolved by consensus between the two reviewers and a third independent reviewer. A unanimous decision between the three reviewers was required to include each paper. The references of each included article were screened for other relevant articles for inclusion. One article was found and included.
Data extraction
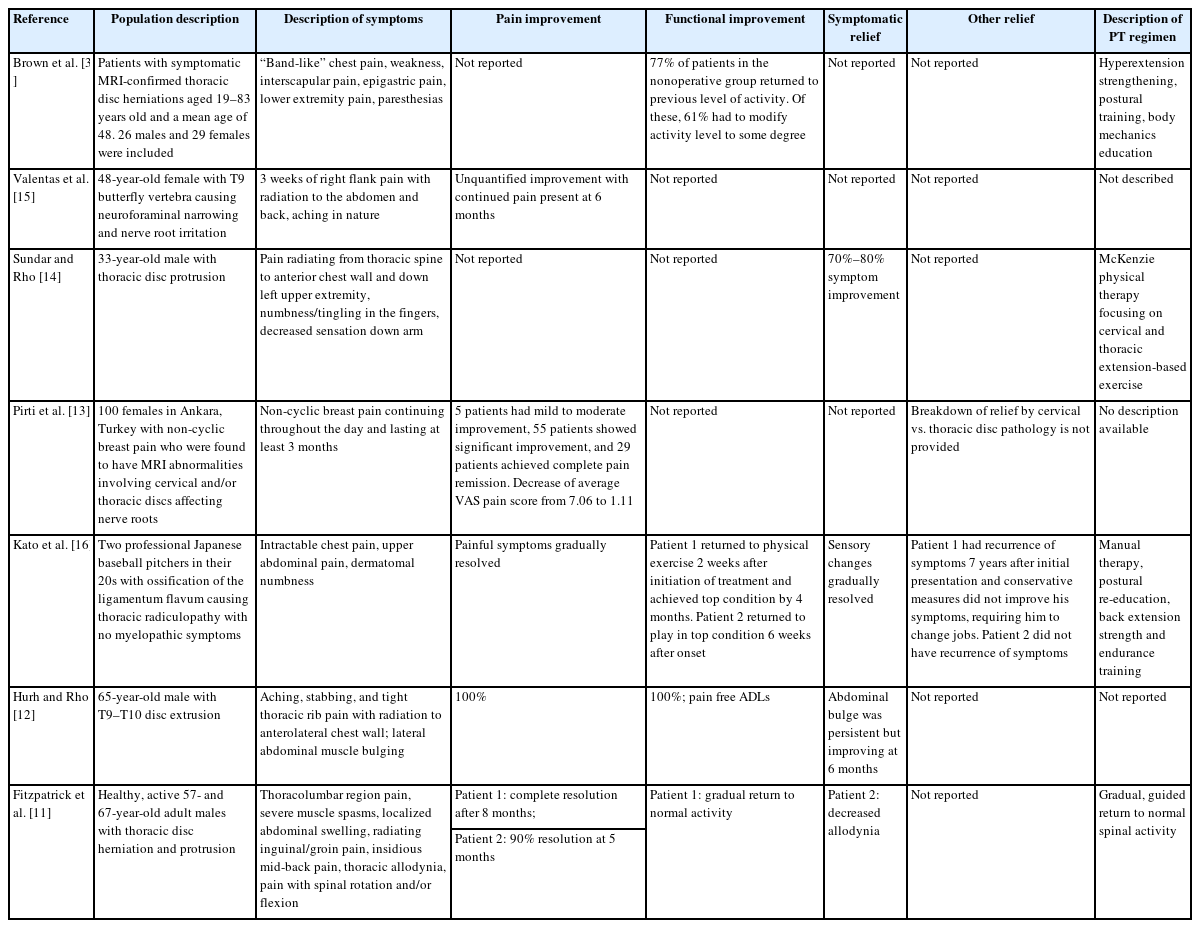
Data were extracted by four independent reviewers (K.A.M., P.T.D., J.P., J.D.H.) utilizing Covidence with each article evaluated in duplicate. Disagreements were discussed between the two reviewers and a unanimous consensus was reached prior to inclusion. The following data were extracted: (1) reference study, (2) population description, (3) description of symptoms, (4) pain improvement, (5) functional improvement, (6) symptomatic relief, (7) other relief, and (8) description of PT regimen (Table 1). Due to the type of selected studies, qualitative data was obtained and summarized in a descriptive manner [6,7].
Risk of bias and methodological quality assessment
Risk of bias was evaluated by four independent reviewers (K.A.M., P.T.D., J.P., J.D.H.) using the National Heart, Lung, and Blood Institute (NHLBI) Study Quality Assessment Tools for observational studies [8]. Case reports were evaluated for risk of bias by the tool put forth by Murad et al. [9] in the British Medical Journal. Each article was assessed by two independent reviewers and consensus was reached between the two when disagreements were found.
Certainty in evidence
Certainty in evidence was evaluated utilizing the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) approach [6,7].
Evidence synthesis
There was a lack of consistent, objective, and well described methods, measures, and reported results within and between the studies included, thus a meta-analysis could not reasonably be performed. The authors instead opted to summarize the findings with a meta-narrative approach (a qualitative systematic-review of mixed-method research). This is indicated when the key clinical factors vary among studies and a variety of methods are used [10].
RESULTS
Characteristics of included studies
A flow diagram of the study selection process is shown in Fig. 1. Seven studies met criteria for inclusion in this review [3,11-16]. None were randomized controlled trials (RCTs) and five were case studies [11,12,14-16]. The remaining two were a prospective cohort study and a retrospective cohort study [3,13]. Patient characteristics are described below in the meta-narrative of included studies.
Risk of bias and methodological quality assessment
The overall study quality assessment demonstrated three studies had “good” quality [12,14,16], one had “fair” quality [11], and three had “poor” quality of evidence [3,13,15] using the NHLBI Study Quality Assessment Tool for Observational Studies (Figs. 2-4) [8,9,17]. Only one of the case studies demonstrated a challenge/rechallenge phenomenon, and none of them had any dose response effect recorded. For the cohort studies identified, statistical evidence and blinding was lacking, exposures were measured only one time, and adjustments were not made for many possible confounding variables. Additionally, sample size justification, objective outcome measures, and properly described PT regimens were lacking across all included studies.
Certainty in evidence
GRADE was applied to the primary objective and indicated that the certainty in evidence was “low” to support the sole use of PT to alleviate symptomatic TR. This assessment was primarily made due to imprecision, as 5 out of the 7 included articles were case studies, and risk of bias, as 57% of the included studies were assessed as having less than “good” study quality. A summary of the GRADE criteria selection for each paper and the overall certainty in evidence is provided (Table 2).
Meta-narrative of included studies
Pirti et al. [13] conducted a prospective cohort study of 139 patients with non-cyclic breast pain. One hundred had normal breast and axillary examinations, negative mammography and/or negative ultrasounds. These 100 patients then received cervical and thoracic spine MRIs. Four patients had no pathologic findings, 96 had evident pathology. Of those with MRI-confirmed pathology, 49 had diffuse cervical-level annular bulging and 47 had cervical disc protrusions. Twelve of 47 also had a thoracic disc protrusion causing thoracic nerve root impingement. All 96 patients received PT that was not specifically described. The authors’ main outcome measure was post-intervention visual analogue scale (VAS). Average VAS at initial examination was 7.06. Seven patients were excluded due to non-compliance with PT. At month 3, 5.6% of patients showed mild-to-moderate improvement, 61.7% showed significant improvement, and 32.5% achieved complete pain remission. Average VAS at month 3 was 1.11. Data stratified by cervical vs. cervical and thoracic disc protrusion was not provided.
Brown et al. [3] performed a retrospective review of 55 patients with significant thoracic disc herniations causing nerve root impingement on thoracic spine MRI. Interviews were conducted to assess their clinical presentation, treatment, and return to activity. They found that 67% of patients experienced an early symptom of anterior band-like chest pain while muscle weakness was observed in 16%. Lesser common symptoms included interscapular pain (8%) and epigastric pain (4%). The operative group (27%) eventually underwent surgery. Over half of the patients who required surgery (55%) had disc herniation below the T9 level, whereas the non-operative group showed a higher frequency of disc herniation between T6–T9 (48%). Differences between the two groups in terms of disc hydration, degree of herniation, number of herniated discs, or level of herniation were not significant. The non-operative group sought treatments including rest, nonsteroidal anti-inflammatory medications, and PT regimens consisting of hyperextension strengthening, postural training, and proper body mechanics education. Duration of PT regimens were not specified. These 77% of patients in this group were able to return to their previous level of activity by the final follow-up visit. They concluded that patients can effectively manage symptomatic TR from disc herniations with rest, medication, and structured PT.
Fitzpatrick et al. [11] presented a case study of two male patients, ages 57 (patient 1) and 67 (patient 2), who developed thoracolumbar pain, muscle spasms, local abdominal swelling, and thoracic allodynia. Both had TR identified by thoracic spine MRI. The TR for patient 1 was caused by an extraforaminal disc protrusion while the TR for patient 2 was caused by foraminal and paramedian disc protrusion with concurrent facet joint arthropathy and small anterior osteophyte complex. Each completed a course of PT, which was not specifically described. Patient 1 experienced symptom resolution at month 8 while patient 2 experienced 90% symptom resolution at month 5.
Hurh and Rho [12] described a case study of a 65-year-old male who had a two-week history of radiating thoracic rib pain into his anterolateral chest wall and lateral abdominal muscle bulging. A thoracic spine MRI identified a T9 radiculopathy caused by T9–T10 lateral foraminal disc extrusion. He completed a course of PT with complete resolution of his pain and improvement in his abdominal bulge by month 6. The regimen of PT was not specifically described.
Kato et al. [16] reported a case study of two Japanese male professional baseball pitchers, ages 22 (patient 1) and 27 (patient 2), who developed chest and upper abdominal pain, as well as numbness. Thoracic spine MRI revealed TR caused by ossification of the ligamentum flavum. Each patient underwent a course of PT described as “manual therapy, postural re-education, and exercise therapy aimed at minimizing thoracic kyphosis-induced spinal loading by increasing the strength and endurance of the back extensors.” The pain and sensory symptoms gradually resolved. Patient 1 returned to play 6 weeks after onset; this patient did not have documented recurrence of symptoms. Patient 2 returned to exercise 2 weeks after initiation of PT and had symptom resolution by month 4. However, 7 years after the initial presentation he did experience symptom recurrence.
Sundar and Rho [14] presented a case study of a 33-year-old male with left-sided chest wall and left upper extremity paresthesia. Thoracic spine MRI revealed a left paracentral T3–T4 disc protrusion with superior migration which impinged the right half of the spinal cord causing a leftwards shift of the cord, resulting in a TR. The patient started McKenzie method PT with a focus on cervicothoracic extension-based exercises. His symptoms decreased by 70%–80% following 10 sessions.
Valentas et al. [15] presented a case study of a 48-year-old female who presented with radiating right flank pain to the abdomen and back. Gastrointestinal or respiratory etiology was ruled out. Thoracic spine MRI showed right T8–T9 neural foraminal narrowing and a T9 butterfly vertebra, causing a right T8 radiculopathy. She was started on nortriptyline, tizanidine and began a course of PT. The PT regimen was not specifically described. The patient’s symptoms had improved by month 6.
Overall, 74 patients were included in this systematic review. Seventy-one had symptoms produced by a thoracic disc protrusion, 2 by ossification of the ligamentum flavum, and 1 by a T9 butterfly vertebra causing neuroforaminal narrowing.
DISCUSSION
This systematic review analyzed the efficacy of participating in a structured, supervised PT program on symptomatic TR. Seven studies were included: 5 case studies, 1 prospective cohort study, and 1 retrospective cohort study. A total of 74 patients with TR were treated with PT prior to any advanced procedures. Although the level of evidence is poor, all studies showed improvement in or resolution of the TR symptoms.
The uncommon diagnosis of TR may elude physicians unfamiliar with its presentation, leading to misdiagnosis, unnecessary procedures, and increased healthcare costs [18]. Given the variability in presentation and etiology, it is essential for a clinician to thoroughly evaluate the patient before arriving at a diagnosis of TR. Diagnosing TR can be challenging due to the complex anatomy, limited procedural access to the thoracic spine, and overlap in symptoms with more common etiologies, such as cardiac, lung or gastroenterological pathologies [2,18]. To differentiate the pathologies, a careful history and physical examination may reveal paraspinal tenderness, dermatomal pain and sensory abnormalities, absent or asymmetric superficial abdominal reflexes, or bulging in the musculature of the affected side, also known as a pseudohernia. These findings can prompt consideration for obtaining MRI; however, specific clinical criteria for diagnosis have not been established [11]. MRI is valuable for assessing the etiology of anatomic compression of thoracic nerve roots or the presence of nerve root T2 hyperintensity in neural damage [1,2]. MRI can also identify the presence of myeloradiculopathy where both the nerve roots and spinal cord are involved. Prompt diagnosis is crucial as the presence of myelopathy can increase patient morbidity [1].
This systematic review highlights that TR presents as a dermatomal pattern of one or more symptoms, such as pain, paresthesia, allodynia, or numbness. This may manifest in the abdomen, flank, chest, back or even breast. Movement may exacerbate the symptoms. Many described an asymmetric abdominal bulge or swelling, representing truncal muscle weakness. Thoracic spine MRI identified the TR in every case.
The most common radiculopathy is symptomatic lumbosacral radiculopathy (LSR) which is seen in 3%–5% of the population and 12%–40% of those experiencing low back pain [19]. A common conservative treatment algorithm for LSR includes patient education, physical activity, and structured PT. If conservative treatment fails, the next step is referral to a specialist to decide between an epidural steroid injection versus surgical decompression [20]. Between 70%–90% of patients improve by conservative treatment alone [21].
Less common is cervical radiculopathy (CR) which is seen in 0.35% of the population [22]. Recommendations for CR mirror those for LSR with the addition of therapeutic modalities, and cervical traction [22,23]. Like LSR, approximately 90% of patients improve by conservative treatment alone [22].
TR differs from its neighboring counterparts in part because of unique structural qualities. Unlike the cervical or lumbosacral spine, the thoracic spine is relatively immobile due to the costovertebral and sternocostal joints. Other unique characteristics include kyphosis, reduced intervertebral disc height and volume, increased spinal cord/canal ratio, and more tenuous vascular supply [1,18,21]. Damage to thoracic nerve roots may occur from degenerative changes in the thoracic vertebrae or intervertebral discs, direct compression from trauma or spinal tumors, inflammatory conditions, or even secondary to diabetic radiculoneuropathy. Anatomic and etiologic differences contribute to the determination of efficacious treatments; however, a formal recommendation based on these differences has not been made from the sparse available data. Expert consensus appears to favor a similar treatment algorithm to CR and LSR. Conservative treatments include PT, weight loss, and mindfulness [1,18]. Data is also sparse on more interventional treatments, such as epidural steroid injections or surgical decompression [24,25].
Limitations
TR appears to be a relatively rare–or at least rarely identified–condition, and this systematic review is limited by the relatively low number of studies (n=7) and included patients (n=74) as well as the fact that there were no randomized control trials found in the literature. These 71% of the studies included were 1–2 patient case studies. Most of the case study patients were male. Many of the studies lack thorough descriptions of the utilized PT programs, outcomes, follow-up periods, and therapy settings which makes replication and clinical applicability difficult. Since no studies included a control group and we excluded studies only if patients underwent advanced interventional procedures, it is difficult to know whether patient improvement was a direct result of PT or some other part of conservative treatment, such as time, rest, or oral medications. The types and length of PT regimens varied widely across the included studies. This review was limited to results in English; relevant studies in other languages may have been excluded. Finally, the inclusion criteria of requiring an MRI-confirmed TR may have been too stringent and excluded other pertinent symptomatic TR studies.
CONCLUSION
Per GRADE, there is low certainty in the evidence to support the use of PT as the sole conservative treatment for symptomatic TR with more than half of the studies (n=4) having less than “good” study quality. This review was limited by a paucity of studies (n=7), of which 71% were case studies. Additionally, few studies (n=3) detailed what PT protocol was used in treatment, making clinical applicability difficult. However, all studies reported pain or functional improvement following a regimen of PT for TR. From the limited number of included studies in this systematic review, conservative treatment led by a PT regimen may help to alleviate symptomatic TR. Further intervention controlled RCTs are needed to strengthen the current literature and establish the efficacy of PT as a conservative treatment for TR. This systematic review highlights the need to define the optimal interventions and the duration of PT treating of TR.
Notes
CONFLICTS OF INTEREST
No potential conflict of interest relevant to this article was reported.
FUNDING INFORMATION
None.
AUTHOR CONTRIBUTION
Conceptualization: Mostert KA, Buus RJ, Prideaux C. Methodology: Mostert KA, Meiling J, Gerberi D, Prideaux C. Formal analysis: Mostert KA, Perera J, Dens Higano J, Davis PT, Meiling J. Project administration: Mostert KA. Visualization: Mostert KA, Meiling J. Writing – original draft: Mostert KA, Perera J, Dens Higano J, Davis PT. Writing – review and editing: Mostert KA, Meiling J, Buus RJ, Prideaux C. Approval of final manuscript: all authors.
SUPPLEMENTARY MATERIALS
Supplementary materials can be found via https://doi.org/10.5535/arm.23136.
Supplementary Table S1.
Full search strategies