- Search
| Ann Rehabil Med > Volume 45(2); 2021 > Article |
|
Abstract
Objective
Methods
Results
AUTHOR CONTRIBUTION
Conceptualization: Kim C, Jang JH. Methodology: Kim C, Jang JH. Formal analysis: Jang JH, Song JH, Choi HE. Project. Administration: Kim C, Kim BY. Visualization: Kim C, Choi HE. Writing - original draft: Jang JH. Writing вҖ“ review and editing: Kim C, Jang JH, Song JH. Approval of the final manuscript: all authors.
Fig.В 1.

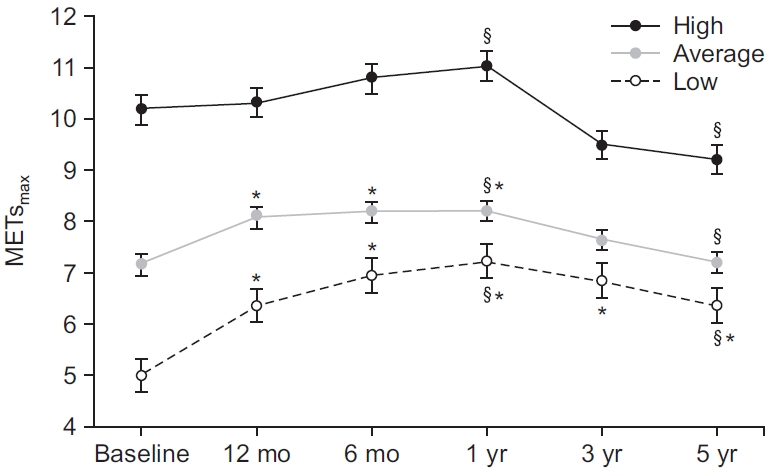
Fig.В 2.
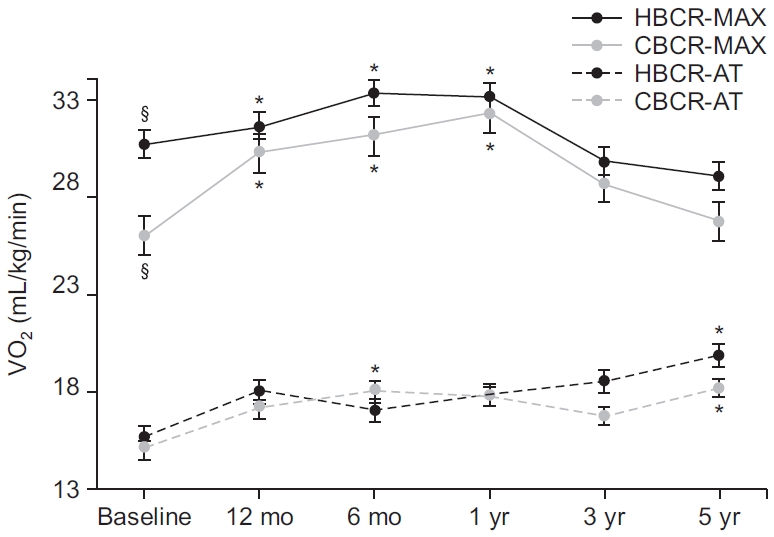
Fig.В 3.
TableВ 1.
| Characteristic | CBCR (n=37) | HBCR (n=41) | p-value |
|---|---|---|---|
| Age (yr) | 63.5Вұ9.3 | 62.1Вұ9.6 | 0.53 |
| Sex | 0.29 | ||
| вҖғMale | 28 | 35 | |
| вҖғFemale | 9 | 6 | |
| BMI (kg/m2) | 24.8Вұ3.6 | 26.2Вұ3.2 | 0.09 |
| LVEF (%) | 58.5Вұ12.7 | 57.9Вұ10.4 | 0.83 |
| Exercise capacity | |||
| вҖғVO2max (mL/kg/min) | 26.4Вұ6.4 | 30.4Вұ7.8 | 0.02* |
| вҖғMETsmax | 7.6Вұ1.8 | 8.9Вұ2.6 | 0.01* |
| вҖғVO2AT | 15.3Вұ4.5 | 15.7Вұ3.4 | 0.73 |
| Smoking history | |||
| вҖғNever | 22 (59.5) | 13 (31.7) | 0.01* |
| вҖғEx-smoker | 6 (16.2) | 10 (24.4) | 0.37 |
| вҖғCurrent | 9 (24.3) | 18 (43.9) | 0.07 |
| Cardiac diagnosis | |||
| вҖғSTEMI | 16 (43.3) | 14 (34.2) | 0.41 |
| вҖғNon-STEMI | 7 (18.9) | 12 (29.3) | 0.29 |
| вҖғUnstable angina | 14 (37.8) | 15 (36.5) | 0.91 |
| Comorbidity | |||
| вҖғHypertension | 21 (56.8) | 21 (56.8) | 0.48 |
| вҖғDiabetes mellitus | |||
| вҖғвҖғNone | 28 (75.7) | 30 (73.2) | 0.80 |
| вҖғвҖғNon-IDDM | 8 (21.6) | 10 (24.4) | 0.76 |
| вҖғвҖғIDDM | 1 (2.7) | 1 (2.4) | 0.35 |
| вҖғDyslipidemia | 13 (35.1) | 12 (29.3) | 0.58 |
| вҖғHeart failure | 4 (10.8) | 2 (4.9) | 0.59 |
| вҖғOthers | 5 (13.5) | 8 (19.5) | 0.66 |
| вҖғNone | 7 (18.9) | 5 (12.1) | 0.95 |
| Revascularization | |||
| вҖғPCI | 35 (94.6) | 39 (95.1) | 0.56 |
| вҖғCABG | 2 (5.4) | 2 (4.9) | 0.91 |
| Number of diseased vessels | 1.57Вұ0.7 | 1.63Вұ0.8 | 0.71 |
| Number of inserted stents | 1.24Вұ0.7 | 1.12Вұ0.6 | 0.39 |
| Number of follow-up CPX test | 9.1Вұ1.8 | 10.0Вұ2.5 | 0.72 |
Values are presented as meanВұstandard deviation or number (%).
CBCR, center-based cardiac rehabilitation; HBCR, home-based cardiac rehabilitation; BMI, body mass index; LVEF, left ventricle ejection fraction; VO2max, maximal oxygen consumption; METsmax, maximal metabolic equivalents; VO2AT, oxygen consumption at anaerobic threshold; STEMI, ST-segment elevation myocardial infarction; IDDM, insulin-dependent DM; PCI, percutaneous coronary intervention; CABG, coronary artery bypass graft; CPX, cardiopulmonary exercise.
TableВ 2.
| CPX results |
CBCR (n=37) |
HBCR (n=41) |
||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Baseline | 12 wk | 6 mo | 1 yr | 3 yr | 5 yr | Baseline | 12 wk | 6 mo | 1 yr | 3 yr | 5 yr | |
| VO2max (mL/kg/min) | 26.4Вұ6.4a) | 30.2Вұ7.6b) | 30.9Вұ8.8b) | 32.0Вұ11.0b) | 28.5Вұ8.0 | 26.4Вұ6.5 | 30.4Вұ7.8a) | 31.4Вұ7.1 | 33.2Вұ7.4b) | 33.1Вұ8.3b) | 29.8Вұ7.2 | 29.0Вұ7.0 |
| METsmax (mL/kg/min) | 7.6Вұ1.8a) | 8.6Вұ2.2b) | 8.8Вұ2.5b) | 9.2Вұ3.1b) | 8.1Вұ2.3 | 7.6Вұ1.9 | 8.9Вұ2.6a) | 9.0Вұ2.0 | 9.5Вұ2.1b) | 9.4Вұ2.4 | 8.5Вұ2.1 | 8.3Вұ2.0 |
| VO2AT (mL/kg/min) | 15.3Вұ4.5 | 17.1Вұ5.0 | 18.2Вұ4.6b) | 17.6Вұ6.8 | 16.5Вұ5.8 | 17.9Вұ4.4b) | 15.7Вұ3.4 | 18.0Вұ4.5 | 17.1Вұ6.5 | 17.9Вұ5.8 | 18.5Вұ5.0 | 19.9Вұ5.1b) |
| RPP3/100 (mmHgвҲҷbpm) | 148Вұ38 | 131Вұ28b) | 131Вұ26b) | 135Вұ33b) | 145Вұ31 | 148Вұ39 | 146Вұ40 | 133Вұ31b) | 136Вұ42b) | 140Вұ27 | 149Вұ39 | 142Вұ32 |
| RPE3 | 10.3Вұ2.4 | 8.7Вұ1.7b) | 9.4Вұ1.7a) | 9.5Вұ1.7a) | 10.0Вұ2.0 | 9.8Вұ1.7 | 9.7Вұ2.8 | 8.3Вұ1.6b) | 8.4Вұ1.9a,b) | 8.6Вұ1.6a,b) | 10.1Вұ2.4 | 12.5Вұ2.0 |
Values are presented as meanВұstandard deviation or number (%).
CPX, cardiopulmonary exercise; CBCR, center-based cardiac rehabilitation; HBCR, home-based cardiac rehabilitation; VO2max, maximal oxygen consumption; METsmax, maximal metabolic equivalents; VO2AT, oxygen consumption at anaerobic threshold; RPP3, rate pressure product at stage 3; RPE3, rate of perceived exertion at stage 3.
TableВ 3.
| CRF | Baseline | 12 wk | 6 mo | 1 yr | 3 yr | 5 yr |
|---|---|---|---|---|---|---|
| High | 10.2Вұ1.9 | 10.2Вұ1.7 | 10.8Вұ1.9 | 11.0Вұ2.6a) | 9.5Вұ2.1 | 9.2Вұ1.6a,b) |
| Average | 7.1Вұ0.6 | 8.0Вұ1.5b) | 8.2Вұ1.4b) | 8.2Вұ1.8a,b) | 7.6Вұ1.6 | 7.2Вұ1.6a) |
| Low | 5.0Вұ0.6 | 6.7Вұ1.5b) | 6.9Вұ1.8b) | 7.2Вұ2.2a,b) | 6.8Вұ1.6b) | 6.3Вұ1.4a,b) |
REFERENCES
- TOOLS







