INTRODUCTION
The estimated prevalence of flat feet is 24% in 6 years old, 44% in 5 years old, and 54% in 3 years old [
1]. Yin et al. [
2] reported the prevalence of flat feet in 6 years old to be 39.5% and agreed that increased body mass index (BMI) and height correlate positively with flat feet. Further, the augmentation in BMI increases the prevalence of postural asymmetry in the anterior, posterior, and lateral planes [
3].
Young school-aged children are particularly prone to postural defects as they undergo a period of development in the spine, in which several factors can impair its normal growth, leading to a change in the shape of the spinal column that causes a shift in the center of gravity [
4]. During postural development, two particularly dangerous periods have been observed in which faulty posture commonly arises: the start of schooling of a child (aged 6–7 years) and puberty [
5]. At ages 4–6 years, a combination of plantar surfaces and somatosensory and visual input appears to be important for postural stability [
6].
However, the relationship between postural asymmetries and disturbances in foot support, such as flat feet, has not been examined in 6 years old, even though the factors above appear to be strictly dependent in primary school students. Good posture is an important topic for growth, beginning in infancy until adolescence.
Considering these premises, asymptomatic flexible flat feet in 6 years old could be associated with specific postural asymmetries. Thus, the aim of this observational study was to determine whether asymptomatic flexible flat feet were associated with specific postural assessments regarding the frontal plane and harmony of spinal alignment in the sagittal plane in 6 years old primary school children.
MATERIALS AND METHODS
Children aged 6 years were included in this cross-sectional observational study [
7] to determine a snapshot of the frequency of flat feet as the dependent variable related to posture.
The subjects were enrolled from the physical medicine and rehabilitation outpatient clinic of the Center of Physical and Rehabilitation Medicine (CUMFeR), University G. D’Annunzio, Chieti, Italy, from January 2017 to September 2017; all 6-year-old children of an entire school complex were recruited consecutively. After receiving information about the study, the parents of the participating children provided written informed consent. The recruitment and evaluation procedures met the Helsinki criteria, and the study’s approval was obtained from the Departmental Committee of the Department of Medical and Oral Sciences and Biotechnologies (DSMOB), University G. D’Annunzio, Chieti, Italy (No. 0417).
The inclusion criteria were age of 6 years, age-appropriate neutral feet or bilateral flat feet, and age-appropriate mental and physical development.
The exclusion criteria were prior surgical intervention, symptomatic or rigid flat feet or asymmetric flat feet, cavus foot, scoliosis, non-compliance, serious medical conditions and neurodevelopmental disorders, ligamentous laxity (Beighton score >6), vestibular and auditory deficits, and visual problems that were corrected with lenses.
Clinical assessment
Two expert physiatrists collected anthropometric data (age, sex, weight, and height); BMI was calculated by dividing body weight by the square of the height (kg/m
2). Compared to BMI, the subject was considered underweight if his BMI was below 18.5, normal weight between 18.5 and 24.9, overweight between 25 and 29.9, and obese at 30 or higher [
8].
Plantar support and foot posture were assessed clinically through a non-quantitative inspection using a podoscope with the Viladot criteria and baropodometry, based on which the clinician determined placement into the neutral foot or flat foot groups [
9-
12].
The podoscope allows for evaluation of the footprint, supplying secondary, indirect information on heel alignment and the toes, and has been used to diagnose flat foot by an expert physiatrist regarding the classification of Viladot [
9,
10]. Generally, in a flexible flat foot, the medial longitudinal arch has full contact with the ground when weight bearing, but the same was normal in a sitting position. On the contrary, in a neutral foot, the longitudinal medial arch while in the sitting and standing position, remains competent and does not collapse to the ground [
13].
Baropodometry (BioMetric Software; Diasu, Rome, Italy) was performed to evaluate foot load symmetry. The static baropodometric test was performed with the subject barefoot, in the standard reference position (bipodalic support and parallel feet, aligned at the heel 5 cm apart, with the arms pending along the body over the platform), with an acquisition time of 5 seconds with their eyes open. In particular, the static baropodometry test was used to calculate the average result of the distribution of foot pressure load, expressed as a percentage of the maximum load. A sensorized mat measured the pressures under the feet and allowed us to identify the center of pressure (CoP), the linear projection of the body’s center of mass (CoM) along the antero-posterior and laterolateral directions. This examination was performed to evaluate the symmetry of the load between the right and left feet, reporting the following parameters: left and right foot static load (FSL), the latero-lateral direction of the body’s center of pressure (CoP X), and the anteroposterior direction of the body’s center of pressure (CoP Y). The average of the results of three consecutive measurements with 10 minutes of rest from one to another was considered [
9].
A clinical postural examination was performed in both the frontal and sagittal planes. For the evaluation postural alignment in the frontal plane, we considered the following lines of symmetry: bis-acromial line, the bisiliac line, and triangles of size. In physiological conditions (good posture), these lines must be parallel to each other and aligned with the two hemisomes [
14]. The following clinical values were collected for the frontal plane: the position of the shoulders (right and left shoulder up), symmetry/asymmetry of the waist (triangle of size), and the position of the anterior-superior iliac spine (ASIS; right and left up). Moreover, knee alignment was determined by measuring the intermalleolar distance, with the use of a ruler, graduated in centimeters. Children were measured in the orthostatic position with observation in a postero-anterior direction view, as recommended in the literature. The distance of ≥8 cm between the intermalleolar was considered as an indicator of valgus knees, and the distance of ≥5cm between the intercondylar distance as varum knees [
12].
For the sagittal plane, the position of the head and spine curvature with respect to the plumb line was recorded considering these parameters: anteposed head, dorsal hyperkyphosis, lumbar hyperlordosis, lumbar hypolordosis, and dorsal hypokifosis. Considering the sagittal profile, the distance from the plumb-line was measured at the spinous processes of C7, T12, and L3 [
15,
16].
These measurements are based on the recent Italian Ministry of Health document of 2017 [
17].
Statistical analysis
Descriptive statistical analyses were performed for continuous quantitative variables and mean±standard deviation (SD) was reported; non-continuous quantitative and qualitative (such as sex and BMI) variables were transformed into dichotomous variables and expressed as percentages or frequency. Qualitative variables were also described using percentages and frequencies.
The univariate analysis considered flat feet as the dependent variable. To determine the association between flat feet and qualitative variables, the chi-square test (χ2) or Fisher exact test was applied. Fisher exact test was adapted to 2×2 tables per the conditions of applicability: no more than 20% of the expected counts is less than 5, and all individual expected counts are 1 or greater.
Significant differences in the mean values of quantitative variables (such as CoP, weight, height, and foot load) between the flat feet and non-flat feet groups were analyzed using the Student t-test for independent samples with equal variance (when the distribution was normal) or the Mann-Whitney U-test. Normal distribution was analyzed by the Kolmogorov-Smirnov test.
A logistic multivariate regression model was used, considering the condition “flat foot” as the outcome, and variables with p>0.150 in the univariate analysis were included as covariates.
Stepwise regression with backward elimination was used, and the goodness of fit of the model was assessed by the Hosmer-Lemeshow test. The significance level for all analyses was set to p<0.05. SPSS version 25 for Windows (IBM, Armonk, NY, USA) was used for all analyses.
The following conditions were assumed to assess the sample size: a level of significance of 95% and a power of the study of 80% with the hypothesis that the presence of flexible flat feet decreased in 6-year-old children, suggesting that ages 3–6 years may be a critical period of development in the medial longitudinal arch: the prevalence of flat feet in the studied population of children is n=57 [
2].
RESULTS
One hundred eighty-three subjects were enrolled and 19 subjects were excluded: 14 due to a failure to meet the inclusion criteria and 5 who declined to participate. One hundred sixty-four subjects were allocated into two groups: 57 with flexible flat feet and 107 with neutral feet.
Table 1 shows the clinical and postural assessments of the subjects. Most subjects were boys (n=96; 58.5%). The prevalence of flexible flat feet was 34.8%. Based on BMI, 98 subjects were normal-weight (59.8%), 43 (26.2%) were overweight, and 23 (14%) were underweight.
As reported in
Table 1, using the static baropodometry test, the mean CoP X was -5.69±10.89, and the mean CoP Y was -24.10±12.86, with a mean difference in load between left and right foot of 5.79 (% of load). With regard to the differences in mean CoP between those with and without flat feet, only CoP Y was significant (p=0.028).
In addition, using a univariate analysis with flat feet as the independent variable, there was no significant difference between the case and control groups (
Table 2).
Moreover, by regression analysis and the Hosmer-Lemeshow test, the covariable BMI-overweight had an odds ratio (OR) of 2.30 (95% confidence interval [CI], 1.11–4.76), and CoP Y had an OR of 1.03 (95% CI, 1.00–1.05) regarding flat feet (
Table 3).
DISCUSSION
As discussed previously, flat feet are one of the most common foot disorders, influencing performance of the foot and affecting the alignment of the ankle, knee, and hip joints and postural stability [
6]. Additionally, the foot arch index, as measured in a static position, could be a functional index that predicts dynamic foot functions while walking. The foot arch influences the pressure distribution under the foot: children with flat feet might shift their body weight to a more medial foot position when walking and could be at a greater risk of soft tissue injury in this area [
18].
In Caucasian children aged 6 years, the prevalence of flat feet was 34.8%, slightly higher than some groups [
1] but consistent with Yin et al. [
2]; in particular, using the baropometric test, CoP Y was altered in the flat feet group (
Table 2). CoP X and CoP Y are decompositions of the CoP with respect to the X-axis (frontal plane) and the Y-axis (sagittal plane): the referential OXY (see
Fig. 1) originates from the center of gravity (COG) of the support polygon. The CoP that coincides with COG arises physiologically in the anatomical position, in which the COG lies approximately anterior to the second sacral vertebra. This line of gravity is important to understand and visualize when determining a person’s ability to successfully maintain balance. When the line of gravity falls outside the base of support, then a reaction is needed to maintain balanced [
19]. These data confirman association betweenthe flattening of the plantar arch with a displacement of CoP Y, which is more posterior than in aneutral foot, in those with flat feet.
Our data show how in flat feet, regarding the sagittal plane, there is an increased load on the hind foot, especially a more back-facing CoP Y, which may indicate functionally less dynamic foot support (
Fig. 1). Also, Holowka et al. [
20] underlined that there are differences in the CoP characteristics between the foot postures (flat foot, normal foot, etc.), which may represent different mechanisms to generate force to facilitate forward progression of the body during gait propulsion phases.
It would seem as if subjects with flat feet had the tendency to be less propulsive and slower than those with normal feet that would be associated with back-facing CoP Y.
Children with flat feet have different static stability, as reported by Kim et al. [
21], who reported the absence of a relationship between static and dynamic stability in adults and that subjects with flat feet have a significantly greater CoP maximum displacement and standard deviation in the antero-posterior direction than those with normal feet.
Further, as shown in
Table 2, there were no significant differences in age with respect to the presence of postural growth disharmony, such as head and spine alignment in the sagittal plane, plumb line, shoulder and pelvis rotation, genu varum and valgus, and asymmetries of the waist triangle with respect to the frontal plane. In addition, the prevalence of flat feet was greater in males, as reported in Yin et al. [
2]. Our results show that flat feet are more common in overweight subjects, and thus, control of the diet should be part of early clinical preventive measures.
The limitations of this study include the lack of intertester or intratester reliability studies on pedobarometry examinations. Nevertheless, footprint evaluation remains an inexpensive, fast, simple, and non-invasive method that can be used effectively for screening and follow-up studies.
In addition, another limit was that the causal relationship between variables cannot be explained as it is a cross-sectional study.
Thus, the early detection of flat feet could allow timely rehabilitative intervention, preventing structural alterations in plantar support in adulthood and postural alterations.
In conclusion, also considering the limitations of this cross-sectional study regarding the postural variables and flat feet outcome, that was simultaneously assessed, and then, there was no possibility to evidence a temporal relationship between them, good posture remains an important indicator of musculoskeletal health in children during growth.
Specifically, in 6 years old, our data did not indicatean association between flat feet and postural assessment likely because the musculoskeletal system is ductile and modifiable in this age group and, even where present, postural disharmony is not structured yet. However, it is important to point out that the treatment of flat feet is indicated only in cases where 6-year-old children have pain and disability. Generally, conservative therapeutic options are used, such as orthotic devices, although in even more complex and refractory cases the only solution is surgery [
22].
Moreover, postural evaluation and instrument-based screens such as baropodometry remain an important step to prevent and to intercept some asymmetry imbalances for future postural alterations that usually occur together with flat feet to start the most appropriate corrective rehabilitation treatment early.
CONFLICTS OF INTEREST
No potential conflict of interest relevant to this article was reported.
AUTHOR CONTRIBUTION
Conceptualization: Saggini R, Bellomo RG. Methodology: Mannocci A, La Torre G. Formal analysis: Mannocci A, La Torre G. Writing – original draft: Paolucci T, Pezzi L. Writing – review and editing: Paolucci T, Pezzi L. Approval of final manuscript: all authors.
Fig. 1.
Static baropodometric test performed with the subject barefoot, in the standard reference position (bipodalic support and parallel feet, aligned at the heel 5 cm apart), with an acquisition time of 5 seconds with open eyes. (A) A footprint of neutral foot and (B) a footprint of flat foot. The gray circle shows the ideal position of the CoM’s linear projection on the ground, and the green circle shows the actual position of the CoM’s linear projection on the ground. CoM, center of mass.
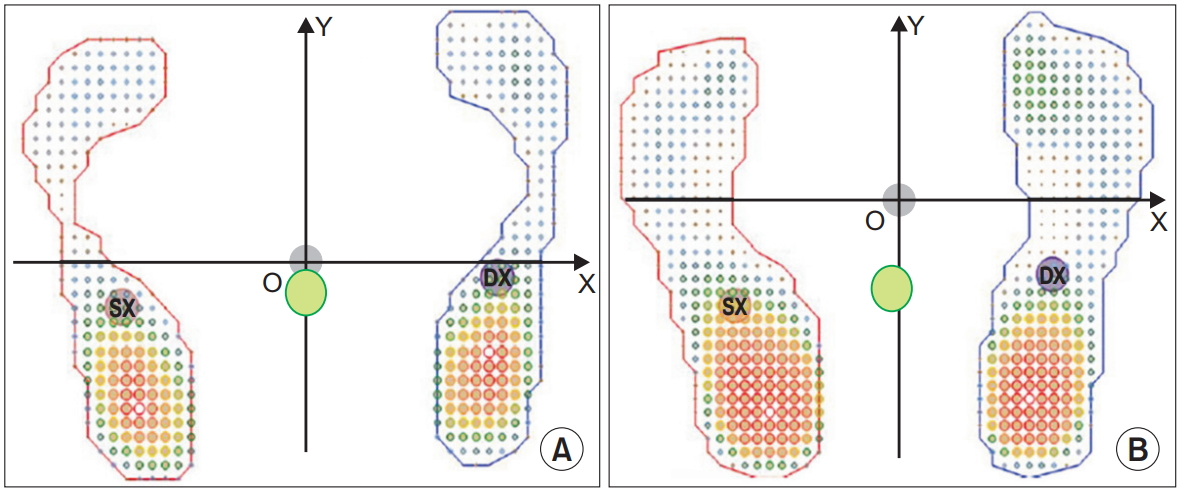
Table 1.
Descriptive statistics and baropodometry variables: frequency analysis, average, and standard deviation (n=164)
|
Characteristics |
Value |
|
Gender |
|
|
Female |
68 (41.5) |
|
Male |
96 (58.5) |
|
Foot shape |
|
|
Flat foot |
57 (34.8) |
|
Neutral foot |
107 (65.2) |
|
BMI |
|
|
Normal weight |
98 (59.8) |
|
Overweight |
43 (26.2) |
|
Underweight |
23 (14) |
|
Postural evaluation |
|
|
Genu valgus |
38 (23.2) |
|
Genu varum |
12 (7.3) |
|
Anteposed head |
23 (14) |
|
Dorsal hyperkyphosis |
14 (8.5) |
|
Lumbar hyperlordosis |
38 (23.2) |
|
Lumbar hypolordosis |
43 (26.2) |
|
Dorsal hypokyphosis |
45 (27.4) |
|
Right shoulder up |
58 (35.4) |
|
ASIS right up |
56 (34.1) |
|
Left shoulder up |
28 (17.1) |
|
ASIS left up |
35 (21.3) |
|
Plumb line |
24 (14.6) |
|
Asymmetry of the right triangle of the size |
66 (40.2) |
|
Asymmetry of the left triangle of the size |
17 (10.4) |
|
Baropodometry testa)
|
|
|
Left-FSL |
52.89±7.72 |
|
Right-FST |
47.10±7.72 |
|
CoP X |
-5.69±10.89 |
|
CoP Y |
-24.10±12.86 |
Table 2.
Analysis between groups (univariate analysis varied for the flat foot variable)
|
Variable |
Neutral foot |
Flat foot |
p-value |
|
Gender |
|
|
0.381a)
|
|
Female |
47 (69) |
21 (31) |
|
|
Male |
60 (63) |
36 (37) |
|
|
Genu varu |
|
|
0.220b)
|
|
Yes |
10 (83.3) |
2 (16.7) |
|
|
No |
97 (63.8) |
55 (36.2) |
|
|
Genu valgus |
|
|
0.140a)
|
|
Yes |
21 (55.3) |
17 (44.7) |
|
|
No |
86 (68.3) |
40 (31.7) |
|
|
Anteposed head |
|
|
0.635a)
|
|
Yes |
14 (60.9) |
9 (39.1) |
|
|
No |
93 (66) |
48 (34) |
|
|
Dorsal iperkyphosis |
|
|
0.937a)
|
|
Yes |
9 (64.3) |
5 (35.7) |
|
|
No |
98 (65.3) |
52 (34.7) |
|
|
Lumbar iperlordosis |
|
|
0.140a)
|
|
Yes |
21 (55.3) |
17 (44.7) |
|
|
No |
86 (68.3) |
40 (31.7) |
|
|
Lumbar hypolordosis |
|
|
0.725a)
|
|
Yes |
29 (67.4) |
14 (32.6) |
|
|
No |
78 (64.5) |
43 (35.5) |
|
|
Dorsal hypokyphosis |
|
|
0.217a)
|
|
Yes |
26 (57.8) |
19 (42.2) |
|
|
No |
81 (68.1) |
38 (31.9) |
|
|
Right shoulder up |
|
|
0.188a)
|
|
Yes |
34 (58.6) |
24 (41.4) |
|
|
No |
73 (68.9) |
33 (31.1) |
|
|
ASIS right up |
|
|
0.221a)
|
|
Yes |
33 (58.9) |
23 (41.1) |
|
|
No |
74 (68.5) |
34 (31.5) |
|
|
Left shoulder up |
|
|
0.907a)
|
|
Yes |
18 (64.3) |
10 (35.7) |
|
|
No |
89 (65.4) |
47 (34.6) |
|
|
ASIS left up |
|
|
0.947a)
|
|
Yes |
23 (65.7) |
12 (34.3) |
|
|
No |
84 (65.1) |
45 (34.9) |
|
|
Plumbe line |
|
|
0.277a)
|
|
Yes |
18 (75) |
6 (25) |
|
|
No |
89 (63.6) |
51 (36.4) |
|
|
Asymmetry of the right triangle of the size |
|
|
0.754a)
|
|
Yes |
44 (66.7) |
22 (33.3) |
|
|
No |
63 (64.3) |
35 (35.7) |
|
|
Asymmetry of the left triangle of the size |
|
|
0.261a)
|
|
Yes |
9 (52.9) |
8 (47.1) |
|
|
No |
98 (66.7) |
49 (33.3) |
|
Table 3.
Analysis logistic multivariate regression and Hosmer-Lemeshow test
|
Co-variable |
OR (expB) |
95% CI (min–max) |
|
Gender M/F |
1.194 |
0.599–2.384 |
|
Genum valgus Y/N |
1.501 |
0.688–3.276 |
|
Normal weight |
1 |
- |
|
Low weight |
0.915 |
0.331–2.530 |
|
High weight |
2.306a)
|
1.116–4.763 |
|
CoP Y/N |
1.030a)
|
1.003–1.057 |
|
Hyperlordosis |
0.223 |
0.742–3.601 |
|
Hosmer–Lemeshow test |
0.941 |
- |
REFERENCES
1. Pfeiffer M, Kotz R, Ledl T, Hauser G, Sluga M. Prevalence of flat foot in preschool-aged children. Pediatrics 2006;118:634-9.


2. Yin J, Zhao H, Zhuang G, Liang X, Hu X, Zhu Y, et al. Flexible flatfoot of 6-13-year-old children: a cross-sectional study. J Orthop Sci 2018;23:552-6.


4. Wojtkow M, Szkoda-Poliszuk K, Szotek S. Influence of body posture on foot load distribution in young school-age children. Acta Bioeng Biomech 2018;20:101-7.
6. Shumway-Cook A, Woollacott MH. The growth of stability: postural control from a development perspective. J Mot Behav 1985;17:131-47.


9. Kerr CM, Stebbins J, Theologis T, Zavatsky AB. Static postural differences between neutral and flat feet in children with and without symptoms. Clin Biomech (Bristol, Avon) 2015;30:314-7.


10. Viladot Perice A. New method of statistical investigation of the feet; photopodography. Clin Lab (Zaragoza) 1954;57:114-7.

11. Garcia-Rodriguez A, Martin-Jimenez F, Carnero-Varo M, Gomez-Gracia E, Gomez-Aracena J, Fernandez-Crehuet J. Flexible flat feet in children: a real problem? Pediatrics 1999;103:e84.


13. Sadeghi-Demneh E, Melvin JM, Mickle K. Prevalence of pathological flatfoot in school-age children. Foot (Edinb) 2018;37:38-44.


14. Paolucci T, Piccinini G, Iosa M, Piermattei C, De Angelis S, Zangrando F, et al. The importance of trunk perception during brace treatment in moderate juvenile idiopathic scoliosis: what is the impact on self-image? J Back Musculoskelet Rehabil 2017;30:203-10.


15. Zaina F, Atanasio S, Ferraro C, Fusco C, Negrini A, Romano M, et al. Review of rehabilitation and orthopedic conservative approach to sagittal plane diseases during growth: hyperkyphosis, junctional kyphosis, and Scheuermann disease. Eur J Phys Rehabil Med 2009;45:595-603.

16. Bricot B. Total postural reprogramming. 4th ed. Santa Monica, CA: Dux Lucis Books; 2014.
19. Iodice P, Bellomo RG, Migliorini M, Megna M, Saggini R. Flexible flatfoot treatment in children with mechanical sound vibration therapy. Int J Immunopathol Pharmacol 2012;25:9S-15S.


21. Kim JA, Lim OB, Yi CH. Difference in static and dynamic stability between flexible flatfeet and neutral feet. Gait Posture 2015;41:546-50.










